Ultrasound Guided Sclerotherapy
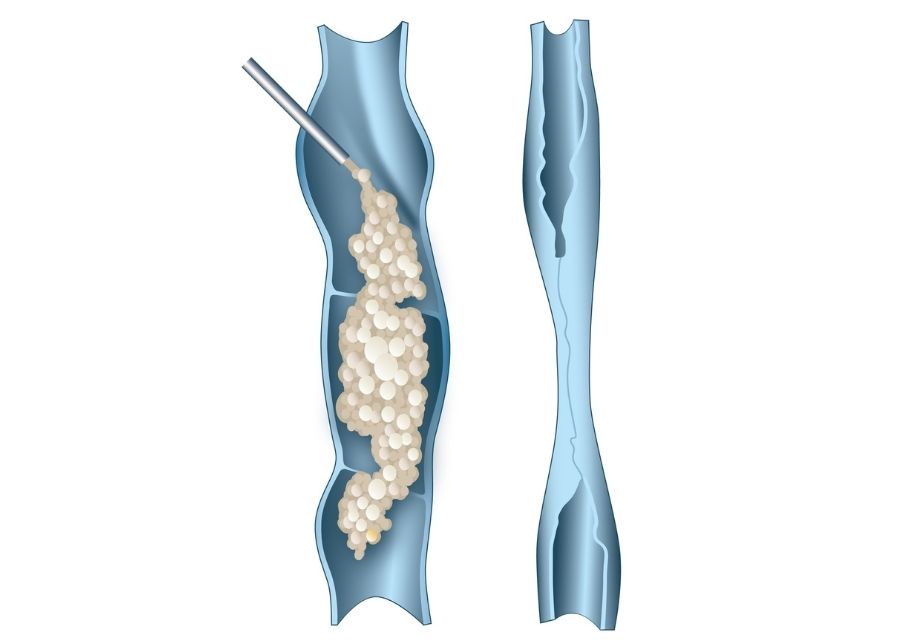

Varicose veins are a global problem with an increasing incidence with age. It is more appropriate to talk about venous hypertension as the underlying pathology with visible varicose veins only one of many disease manifestations.
Varicose eczema, restless and aching legs, ankle swelling, skin damage due to oxygen starvation leading to ulceration and delayed healing are all “signs” of venous hypertension.
The gender spread is about 1/3 men, 2/3 women with venous hypertension occurring in 8% of women aged 20-29, 41% of women aged 50-59 and 72% of women aged 70-79. In men varicose veins occur in 1% aged 30-39, 24% aged 40-49 and 43% aged 70-79.
Risk factors for developing varicose veins include pregnancy, positive family history, occupations involving long periods of standing, obesity and a past medical history of deep vein thrombosis.
There are two venous systems in the lower leg – the deep venous system which lies within the muscle and the superficial venous system which is positioned between muscle and skin.
The deep venous system carries 90+% of the venous return from the legs, i.e. all of the muscle drainage. The superficial venous system drains the remaining structures such as fat, skin and nerves, in addition it serves as a vascular storage and facilitates heat dissipation.
In almost all cases of venous hypertension we are dealing with a pathology of the superficial system, in particular the two main saphenous veins. The Great Saphenous Vein (GSV) which runs from the ankle to the groin up the medial side of the leg, and the Short Saphenous vein (SSV) which runs in the midline posteriorly up the calf. These veins empty into the deep venous system at the Sapheno-Femoral Junction (SFJ) in the groin and the Sapheno-Popliteal Junction (SPJ) behind the knee.
In order for blood to return from the lower limbs against gravity the pumping action of the intra-muscular deep veins is augmented by a series of one-way valves throughout the length of the vein. Varicose veins result through a failure of these valves and blood refluxes back down and out into the superficial venous system and its branches.
These veins subsequently become dilated and tortuous and, if close to the skin, can be seen as visible lumpy varicose veins, but are not always visible. Due to the retrograde flow within these veins, the superficial low pressure system becomes a high pressure system, a condition known as chronic venous hypertension.
As a result of reduced oxygenation of local tissues and leakage of intravascular fluid into the surrounding tissue inflammation and oedema ensues. These then manifest in a variety of symptoms such as swelling, aching, cramping, pain and restless legs. The skin can also become compromised with poor healing, skin pigmentation, venous eczema and venous ulceration. Sometimes a varicose vein can become thrombosed and present as a hot, inflamed and tender area, often misdiagnosed as cellulitis. This superficial venous thrombosis (SVT) has a real risk of progressing to a DVT.
Chronic venous hypertension therefore causes significant morbidity and significantly decreases a patient’s quality of life, even without overtly visible varicose veins.
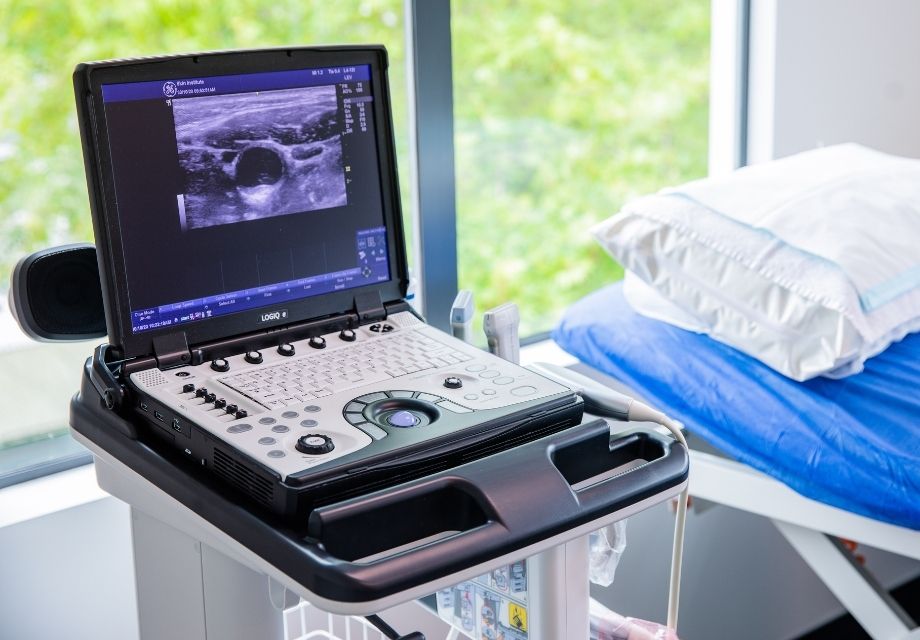
It is essential that all patients have a comprehensive medical assessment and subsequently a lower limb venous mapping with duplex ultrasound. The purpose of this investigation is to map the pattern of venous reflux for each individual patient.
This involves determining where the reflux begins, which veins are involved, where they run and all their associated interconnections. The deep venous system is also checked for reflux or obstruction. With this information we can then proceed to formulating an individualised treatment plan.

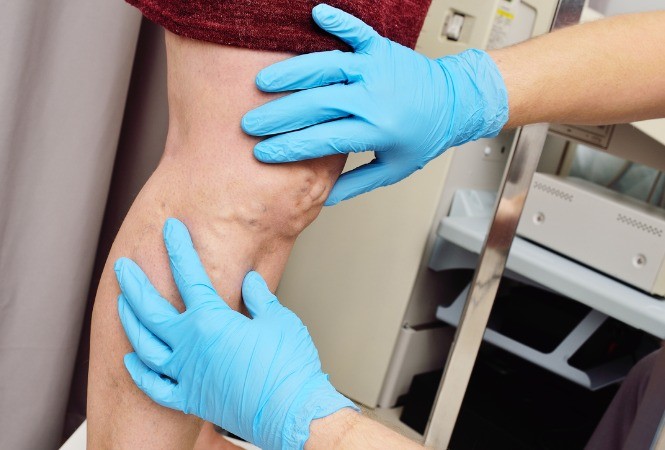
Venous stripping is now an outdated procedure similar to other open access surgery that has been replaced in the last few decades with minimally invasive procedures to great benefit for the patient and the health system in general.
Moving away from “one-off” surgery requiring general anaesthetic and hospitalisation to a less invasive and debilitating model is much more in keeping with the chronic nature of venous hypertension and varicose veins.
Non-invasive procedures removing the need for general anaesthetic and at a much lower risk of complications such as wound breakdown and infections also allows the widening of the eligible population to older patients or individuals with pre-existing conditions putting them at greater risk.
Skin Institute always investigates new procedures and we are currently evaluating endovenous acrylic glue to effect closure of the truncal veins. Whilst this procedure removes the need for local anaesthetic injections some concerns around the longterm effects of acrylic glue remain.

After both Endovenous Ablation and Ultrasound Guided Sclerotherapy patients are fitted with compression stockings and advised on post treatment instructions. This will include daily walking to reduce the small risk of a DVT. The patients will be followed up after 3 months and again several times over the following year. Commonly patients will receive a mixture of Endovenous Ablation and Ultrasound Guided Sclerotherapy to completely treat their varicose vein disease.

Please consider referral of any patients who may have symptoms or signs of varicose veins disease. Large lumpy varicose veins are not always necessarily seen and so if you have any suspicion, we are happy to consult and map any patients. We welcome all your referrals via phone 0800 SKIN DR (754637), Healthlink, Specialist Referrals or Manage My Health. In the South Island, you can refer via ERMS. Alternatively, your patient can directly request an appointment by telephone or through our appointment form on our website.
EDI: skininst